 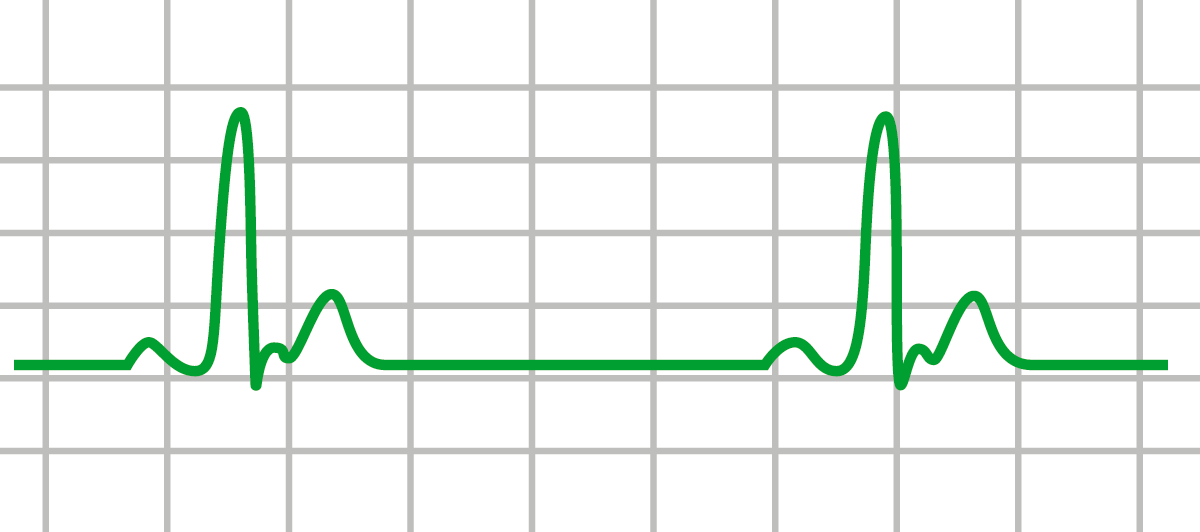
Hypovolemia ( shock), hypoxia, electrolyte imbalance (example high or low potassium), thrombosis, some type of trauma, cardiac disease etc. Causes of Pulseless Electrical Activity (PEA) 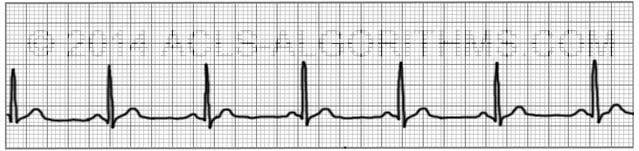
This rhythm is a great example of why you can’t always trust the ECG monitor and must check the patient for yourself. 
However, again when you go to check the patient, they will have NO pulse and be unresponsive. In addition, you may or may NOT see p waves and QRS complex. Immobilized patients, recent surgical procedures (e.g.The organized presentation of this rhythm can vary in that you may see something on the ECG that looks like normal sinus rhythm, sinus bradycardia, sinus tachycardia etc. Post-cardiac surgery, malignancy, post-myocardial infarction, pericarditis, trauma Hypokalemia: alcohol abuse, diabetes mellitus, diuretics, drug overdose, profound gastrointestinal lossesĪlcohol intoxication, significant burns, drowning, drug overdose, elderly patient, endocrine disease, environmental exposure, spinal cord disease, traumaĬentral venous catheter, mechanical ventilation, pulmonary disease (e.g., asthma, chronic obstructive pulmonary disease), thoracentesis, thoracic trauma Hyperkalemia: drug overdose, renal dysfunction, hemolysis, excessive potassium intake, rhabdomyolysis, major soft tissue injury, tumor lysis syndrome Upper airway obstruction, hypoventilation (central nervous system dysfunction, neuromuscular disease), pulmonary diseaseĭiabetes, diarrhea, drug overdose, renal dysfunction, sepsis, shock Significant burns, diabetes, gastrointestinal losses, hemorrhage, malignancy, sepsis, trauma He was transferred to the intensive care unit for further monitoring. Serum magnesium and troponin levels were unremarkable. A stat basic metabolic panel was obtained and confirmed the POC electrolyte derangements. Intravenous (IV) calcium gluconate, IV insulin and dextrose, albuterol nebulization, and 40 mg IV Lasix were administered. Stat point-of-care (POC) electrolytes were obtained, which showed hyperkalemia with a potassium level of 7.2 mmol/L. A stat electrocardiogram (EKG) was obtained and showed peaked T waves in the precordial leads ( Fig. Examination after the achievement of ROSC showed that the patient was responding appropriately to painful stimuli. Return of spontaneous circulation (ROSC) was achieved after 5 min, and normal sinus rhythm was restored. 
A sine wave pattern was seen on the cardiac monitor during CPR ( Fig. A total of two rounds of CPR were performed, and a total of two ampules of 1 mg (1:10,000) epinephrine were administered. The patient was intubated emergently to secure the airway. No other examination was performed during CPR. No spontaneous activity was present, and the patient was pulseless. It showed a pale, elderly appearing male undergoing chest compressions and bag-valve ventilation. Pulse Oximetry: 88% on 100% oxygen with Ambu-bagĪ limited exam was done in the setting of cardiac arrest. Respiratory Rate: Ambu-bagged at ten breaths per min Upon arrival, the bedside nurse was already performing cardiopulmonary resuscitation (CPR), and the attached cardiac monitor showed pulseless electrical activity (PEA).īlood Pressure: 80/40 mmHg while CPR being performed On prompt arrival of the rapid response team, it was noted that the patient was a 69-year-old male with a known history of type 2 diabetes, hypertension, COPD (on 4 L/min of oxygen at home), and tobacco abuse disorder, who was admitted with ST-elevation myocardial infarction and was two days post-coronary artery bypass grafting. A rapid response event was initiated by the bedside nurse for a patient with sudden unresponsiveness. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
